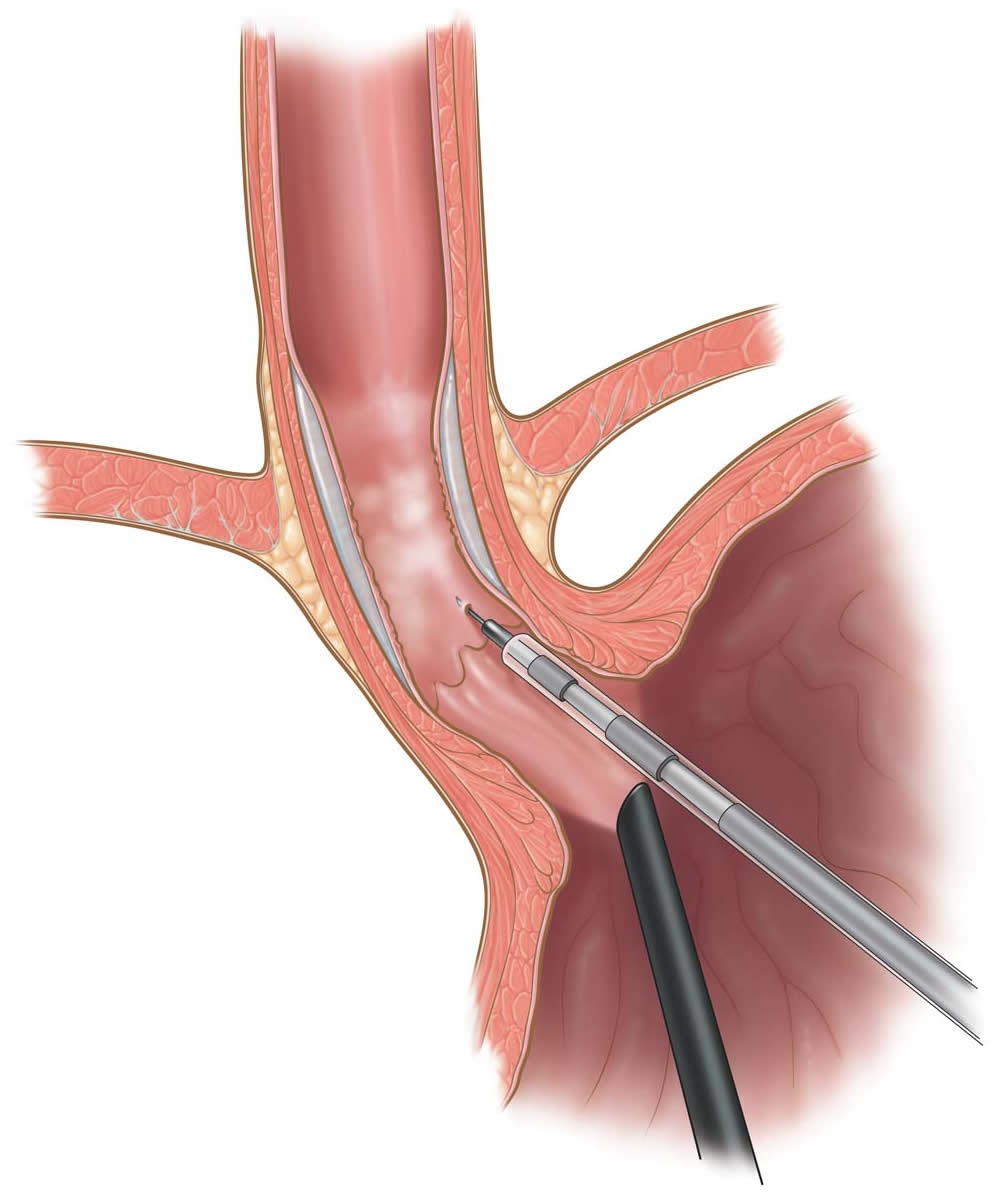
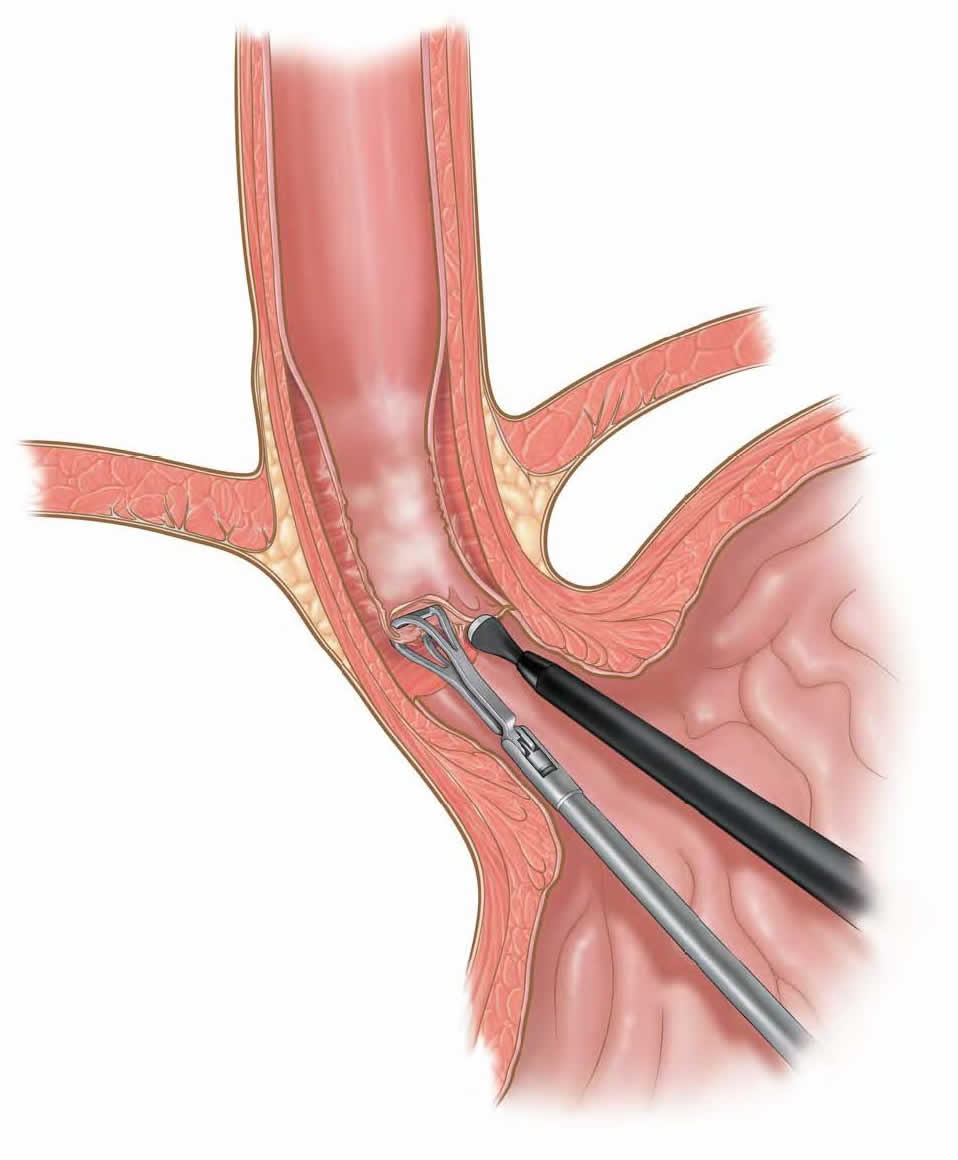
Laparoscopic Transgastric Esophageal Mucosal Resection (removal of esophageal lining)
A. The Condition. You may have a condition in which the lining of your lower esophagus has become precancerous. The medical term for this is “Barrett’s Esophagus with severe dysplasia.” This can be a consequence of years of acid reflux. In order to prevent cancer from developing, the lining of your esophagus will be removed with a laparoscopic operation.
B. Symptoms
- Heartburn (this can be present for years)
- Regurgitation (spitting up)
- Difficulty swallowing
C. Laparoscopic Transgastric Esophageal Mucosal Resection. The surgeon will make about 4-5 small incisions in your abdomen. A port (nozzle) is inserted into one of the slits, and carbon dioxide gas inflates the abdomen. This process allows the surgeon to see inside of your abdomen more easily. A laparoscope is inserted through another port. The laparoscope looks like a telescope with a light and camera on the end so the surgeon can see inside the abdomen. Surgical instruments are placed in the other small openings and used to remove the lining of your esophagus. This is done by first making a small incision in the stomach to access the inside of the esophagus where the lining is. The abnormal lining is placed into a plastic bag, and removed from your abdomen through one of the small incisions. After the lining has been removed, the incision on the stomach is closed with a stapler, and a valve mechanism (fundoplication) is performed to prevent acid reflux. After this has been accomplished, the carbon dioxide is released out of the abdomen through the slits, and then these sites are closed with sutures or staples, or covered with glue-like bandage and steri-strips.
This procedure was performed by Dr. Frantzides for the first time in the world in 2002, and was published in 2004.
D. Nonsurgical Treatment. There are a number of treatment options for precancerous lining of the esophagus; many utilize endoscopy (sticking a tube down your throat). None of the other treatment options treat the underlying disease (acid reflux) as does laparoscopic transgastric esophageal mucosal resection. Your doctors will discuss your treatment options with you to determine which is best for you.
E. Risks. The primary risks of laparoscopic transgastric esophageal mucosal resection are:
Esophageal perforation
Leak at the stomach staple line
Infection of the skin at one of the small ports sites
Postoperative ileus (the intestines slow down/stop working for several days)
F. Expectations
1. Before Your Operation. Laparoscopic transgastric esophageal mucosal resection is usually an elective procedure. The preoperative evaluation might include blood work, urinalysis, abdominal x-rays, upper endoscopy (looking into your esophagus from the throat with a scope), and an abdominal CT scan. You also may have a barium x-ray of your esophagus. If you smoke, then you should stop immediately. If you are taking blood thinners (for example, aspirin, coumadin, Lovenox, or Plavix), then you will need to stop these one week prior to your procedure. You may need an extensive evaluation of your heart and lungs to determine if you are fit for surgery. Your surgeon and anesthesia provider will review your health history, medications (including blood thinners), and options for pain control.
2. Your Recovery. You usually can go home in 2-3 days after a laparoscopic transgastric esophageal mucosal resection. You may have to wait for your bowels to start working. You should avoid foods that give you gas. You also should avoid liquids that can irritate the surgical site, such as alcohol and acidic juices. You may have to adjust your diet to eat smaller, more frequent meals. You will be given medication for pain. You should limit your activity to light lifting (no more than 15 lb) for one month.
3. Call Your Surgeon if you have one or more of the following:
Severe chest or abdominal pain
High fever
Odor or increased drainage from your incision
No bowel movements for three days
G. Pertinent References.
Frantzides CT, Madan AK, Moore RE, Zografakis JG, Carlson MA, Keshavarzian A. Laparoscopic transgastric esophageal mucosal resection for high-grade dysplasia. J Laparoendosc Adv Surg Tech A. 2004 Oct;14(5):261-5.
Kent M, Luketich JD. “Minimally Invasive Esophagectomy.” In: Frantzides CT, Carlson MA, eds. Atlas of Minimally Invasive Surgery. Philadelphia: Saunders Elsevier, 2009.
Frantzides, C.T., Carlson M, Keshavarzian A, Roberts J.; Laparoscopic Transgastric Esophageal Mucosal Resection, Am. J. Surg. 200 (2):305-307,2010
Frantzides, C.T., Roberts J., Welle S., Laparoscopic Esophageal Mucosal Resection for High Grade Dysplasia. Video Atlas of Advanced Minimally Invasive Surgery, Sounders Elsevier pp 55-58; 2013
Frantzides C.T., Daly S. C., Frantzides A. T., Manelis T., Marcinkevicius A., Luu M. B., “Laparoscopic Transgastric Esophageal Mucosal Resection: A treatment option for patients with High-Grade Dysplasia in Barrett’s Esophagus”, Am. J. Surg, 211: 534-536,2016